New funding enables vital research in childhood cancer treatment
Neuroblastoma is a solid-tumour cancer that affects just over 100 children in the UK each year and contributes to 15% of childhood cancer deaths. However, a team of GOSH cancer doctors have now received funding to develop an exciting new surgical technique, which could improve outcomes.
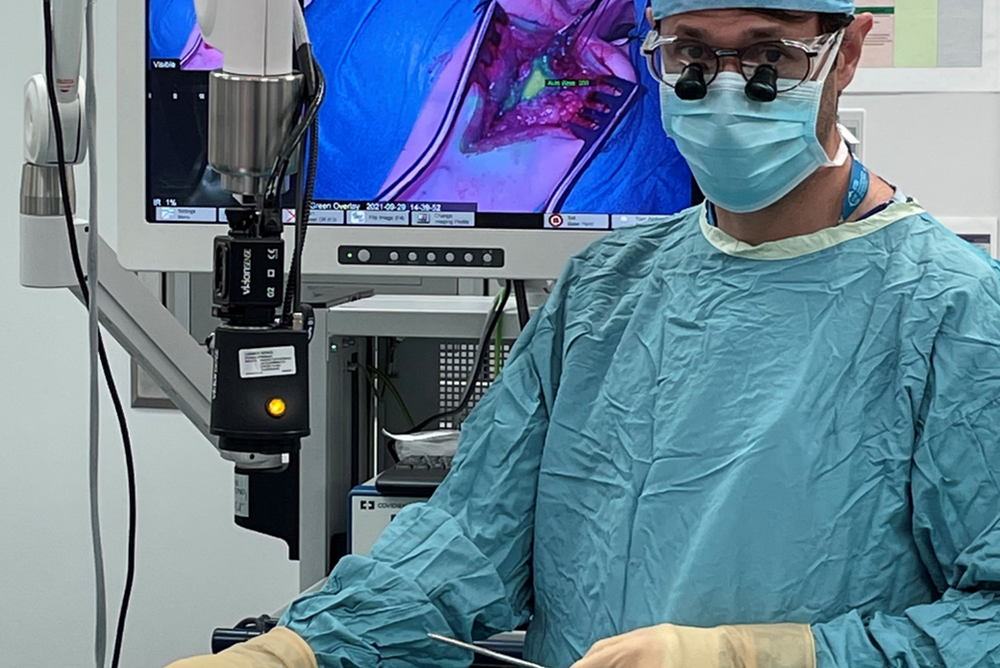
These technological innovations aim to help surgeons precisely see the edges of cancer tissue during an operation, inside the body, using special molecules called fluorophores that ‘light up’ living cancer cells. This will help surgeons remove every piece of the tumour, preventing future spread.
Why is research into neuroblastoma needed?
Neuroblastoma is the second most common solid cancer in children, after brain tumours, and is often aggressive. Despite advances in treatment, it still has a high mortality and around 50% of children with high-risk neuroblastoma will sadly die.
One major weapon against these cancers is surgery to remove the tumour, but current techniques mean the surgery is challenging and doesn’t always remove all of the cancer. The surgeries often take six to eight hours, and the tumours can grow on and around major vessels and organs like the liver and kidneys. Surgeons often struggle differentiating between tumour and healthy tissue, beyond the look and feel of the tissue. This means it is very easy for small pieces of the cancer to be left behind, allowing them to spread at a later date.
New funding for GOSH research team
This team of scientists and doctors at Great Ormond Street Hospital NHS Foundation Trust (GOSH) and UCL Great Ormond Street Institute of Child Health (UCL GOS ICH) have been awarded a £519,000 Wellcome Trust Innovator Award to continue their ground-breaking research using image-guided surgery in childhood cancers.
The team, led by Mr Stefano Giuliani a specialist neonatal and paediatric surgeon at GOSH, involves a multidisciplinary group of experts in the field of children cancer, engineering and novel treatments. Professor of experimental paediatric oncology at ICH, John Anderson, and Professor of biomedical photoacoustics at UCL, Paul Beard, and Dr Gabriela Kramer-Marek from the Institute of Cancer Research, London, and the Royal Marsden Hospital are part of the expert team developing a new platform to remove neuroblastoma more effectively using novel technologies and devices to improve surgical outcomes.
A recent grant will support studies in animals for 2 years, after which, if successful, the team hope to translate the results into a surgical clinical trial.
How could ‘colour-coded’ surgery research improve outcomes for neuroblastoma patients?
In this new project, the team are developing technologies that can help surgeons precisely see the edges of cancer tissue during an operation, inside the body, using special molecules called fluorophores that ‘light up’ living cancer cells.
The fluorophores will be attached to antibodies that specifically target a protein present on the membrane of cancer cells and injected intravenously before an operation. Following, a custom-designed camera will be used to help surgeons visualize the 'glowing' cancer margins.
This will help to improve surgery for children with cancer in three vital ways:
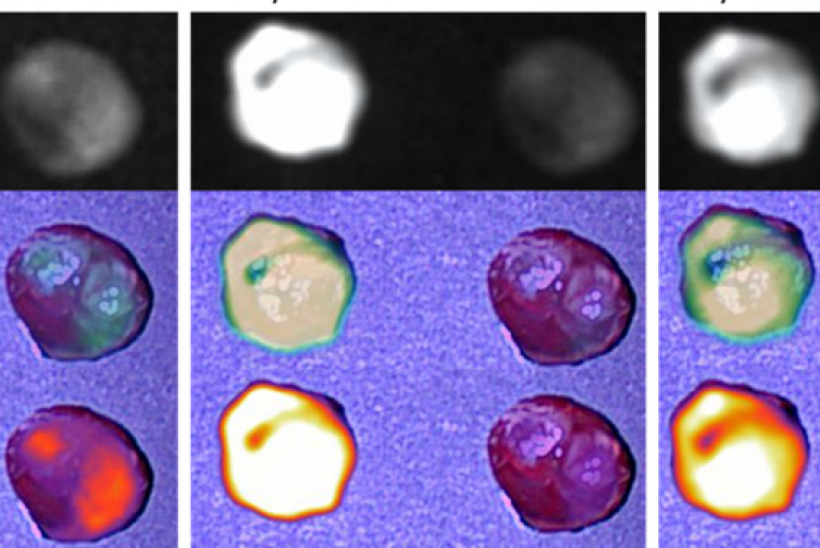
- Tumour visualisation: By ‘lighting up’ tumours, surgeons will be able find the cancer more easily and remove it, avoiding vital organs like the kidney and liver.
- Removal of residual cancer: After the cancer has been located and mostly removed, the surgeons can use an innovative scanner to look for small pieces of the tumour that are left behind. These will be visible as ‘glowing’ spots under the camera.
- Removing ‘invisible’ cancer cells: Once the surgeons have removed all the cancer that they can see with the cameras and scanners, there may still be cancerous cells that are ‘invisible’. The special characteristics of the fluorophore mean that, under a special wavelength of light they will become ‘excited’, giving out energy that can kill nearby cancer cells.
These novel technologies have the potential to make surgery for childhood cancers safer and more effective.